
The overall goal is to provide comprehensive care that addresses the patient’s physical, emotional, and psychological needs to promote healing, prevent complications, and promote recovery. The nursing care planning goals for a patient with a burn injury include pain management, infection prevention, wound care, nutritional support, psychological support, and promoting mobility and rehabilitation. Helping the patient adjust to the changes the injury has imposed is also a priority. The focus is on helping the patient return to a normal injury-free life. This stage starts with the closure of the burn and ends when the patient has reached the optimal level of functioning. The final stage in caring for a patient with a burn injury is the rehabilitative stage. Assessment of central venous pressure gives information regarding the patient’s fluid status. If renal and cardiac functions do not return to normal, the added fluid volume, which prevented hypovolemic shock, can now produce manifestations of congestive heart failure. Alterations in capillary permeability and a return of osmotic pressure bring about diuresis or increased urinary output. The intermediate phase of burn care starts about 48–72 hours after the burn injury. During the emergent phase, the priority of patient care involves maintaining an adequate airway and treating the patient for burn shock. The emergent phase starts with the onset of burn injury and lasts until the completion of fluid resuscitation or a period of about the first 24 hours. The three phases are the emergent phase, intermediate phase, and rehabilitative phase. There are three phases of burn injury, each requiring various levels of patient care. Paying attention and caring for a patient with burns serve as an extraordinary demand to even the most experienced nursing staff because few injuries pose a greater threat to the patient’s physical and emotional well-being. This burn requires skin grafting and prolonged periods of recovery. 
A third-degree burn indicated the destruction of the entire epidermis and dermis and typically involves fat and muscle the skin may be white, charred, or leathery in appearance. The skin may be waxy white in appearance and require grafting or prolonged periods of recovery. A deep second-degree burn indicates destruction of the epidermis and dermis, leaving only the epidermal skin appendages within the hair follicles. Healing is complete but requires extended time to occur. A superficial second-degree burn indicates destruction of the epidermis and the upper third of the dermis it is characterized by pain and blister formation. Healing is complete and occurs within 5 to 10 days. 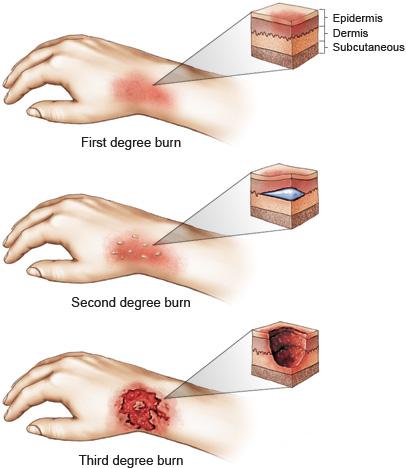
Classifications of the depth of burns include first-degree (partial thickness), second-degree (superficial or deep partial thickness), and third-degree (full-thickness).Ī first-degree burn indicates destruction of the epidermis resulting in localized pain and redness. It’s commonly fatal or permanently disfiguring and incapacitating (both emotionally and physically).īurns are classified according to the depth and extent of the injury. A major burn is a catastrophic injury, requiring painful treatment and a long period of rehabilitation. Scalds from hot liquids and steam, building fires, and flammable liquids and gases are the most common causes of burns. Monitoring Results of Diagnostic and Laboratory ProceduresĪ burn injury is damage to your body’s tissues caused by heat, chemicals, electricity, sunlight, or radiation. Administer Medications and Provide Pharmacologic Support Initiating Patient Education and Health Teachings Providing Wound Care and Improving Skin Integrity Learn about the nursing assessment, nursing interventions, goals and nursing diagnosis for patients with burns in this guide. Use this nursing care plan and management guide to help care for patients with burn injury.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
